When you pick up a prescription at the pharmacy and see a different name than what your doctor wrote, it’s probably a generic drug. These pills look different, cost far less, and often come in plain packaging-but they work just like the brand-name version. So how are they made? It’s not just copying a pill. It’s a precise, heavily regulated science that takes years, millions of dollars, and strict oversight to get right.
Starting with the Original: Reverse Engineering the Reference Drug
Before a single tablet is pressed, manufacturers must fully understand the brand-name drug they’re copying. This drug is called the Reference Listed Drug (RLD). The process begins by breaking it down: what’s the active ingredient? What are the excipients (inactive ingredients like fillers, binders, or coatings)? How is it structured at the molecular level? This isn’t guesswork. It’s analytical chemistry at its most detailed. Companies use advanced tools like mass spectrometry and high-performance liquid chromatography to map out every component. Even tiny differences in particle size or crystal form can affect how the drug is absorbed. For example, if the original uses a specific type of lactose as a filler, the generic must match that particle size-because a slight change can alter how fast the tablet dissolves in your stomach. One pharmaceutical engineer on Reddit shared that a shift in lactose supplier once ruined an entire batch of generic tablets because the new powder didn’t bind properly. That’s why every material is tested and documented before production even starts.The Blueprint: Quality by Design (QbD) and Critical Parameters
Modern generic drug manufacturing doesn’t just follow recipes-it builds a science-based system called Quality by Design (QbD). This framework, developed by the International Council for Harmonisation (ICH), identifies three key elements:- Critical Quality Attributes (CQAs): What must the final product do? For example, the tablet must release 85-115% of the drug within 30 minutes.
- Critical Material Attributes (CMAs): What properties of raw materials matter? Like particle size of the active ingredient or moisture content in the binder.
- Critical Process Parameters (CPPs): What steps in manufacturing affect the outcome? Temperature during drying, pressure during compression, mixing time-all are monitored and controlled.
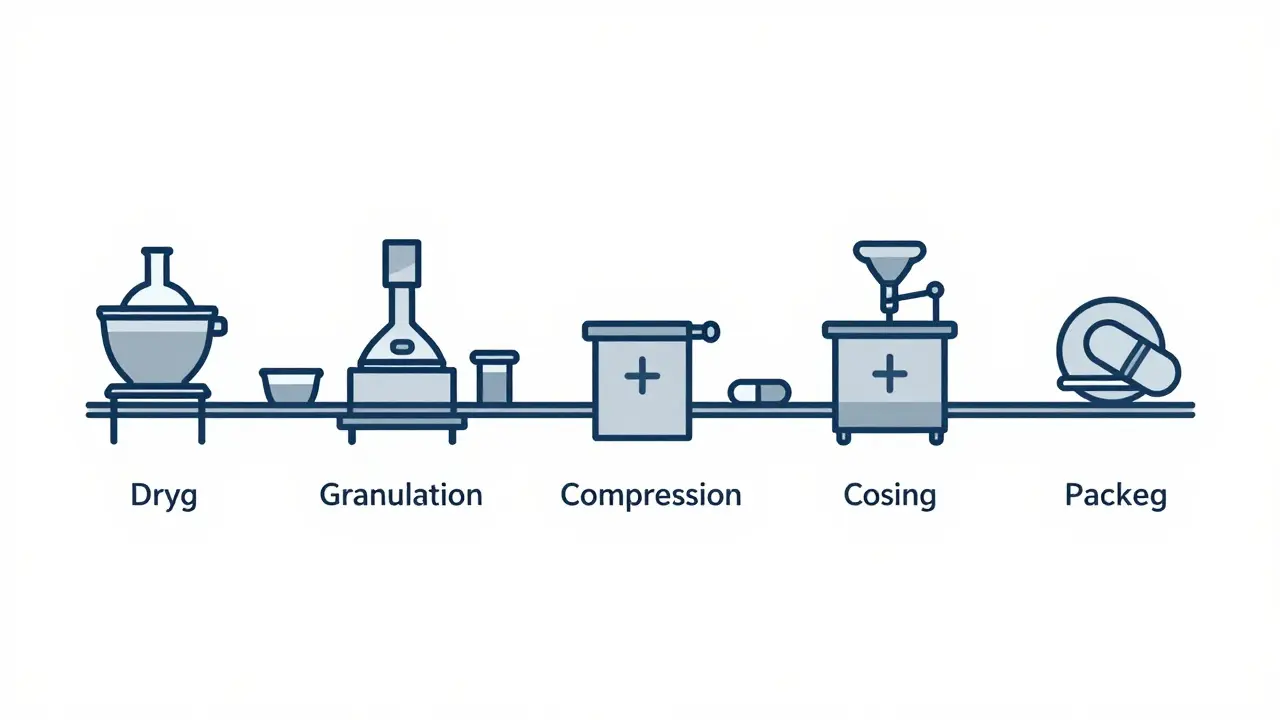
The Seven-Stage Manufacturing Process
Once the blueprint is set, production follows a strict sequence:- Formulation: The active pharmaceutical ingredient (API) is mixed with excipients in precise ratios. Even a 0.5% error in weight can push the drug outside FDA limits.
- Mixing and Granulation: Powders are blended until uniform, then turned into granules (small clumps) to improve flow during compression. Wet granulation uses liquid binders; dry granulation uses rollers to compress powder into sheets.
- Drying: Granules are dried in heated chambers to remove moisture. Too much water? The tablet can degrade. Too little? It crumbles. Humidity in the room is kept between 45-65% to prevent this.
- Compression and Encapsulation: Dry granules are pressed into tablets using high-pressure machines. For capsules, the powder is filled into gelatin shells. Tablet weight must stay within ±5% for pills under 130mg, or ±7.5% for heavier ones.
- Coating: Tablets get a thin outer layer to mask taste, protect from moisture, or control release. Some coatings dissolve in the stomach; others wait until the intestine. This step alone can take weeks to perfect.
- Quality Control: Every batch is tested. Tablets are checked for weight, hardness, dissolution rate, purity, and microbial contamination. Dissolution testing is especially critical-FDA requires the generic to release the drug at the same rate as the brand, within 80-125% of the original.
- Packaging and Labeling: Tablets are sealed in blister packs or bottles with child-resistant caps. Labels must match the brand’s in active ingredient, strength, and usage instructions-but can’t copy the brand’s color or shape. U.S. trademark law prevents generics from looking too similar to avoid confusion.
The Approval Pathway: The ANDA Process
You can’t just start making generic drugs. You need FDA approval through the Abbreviated New Drug Application (ANDA). This is where the process gets its name: “abbreviated” because you don’t repeat the 10-year clinical trials the brand company did. Instead, you prove you’re equivalent. The ANDA has five steps:- Submission: You file 5,000-10,000 pages of data: chemistry, manufacturing, bioequivalence studies, and facility details.
- Bioequivalence Testing: 24-36 healthy volunteers take both the brand and generic drug. Blood samples are taken over hours to measure how much drug enters the bloodstream (Cmax) and how long it stays (AUC). The generic’s values must fall within 80-125% of the brand’s-90% of the time.
- Facility Inspection: The FDA sends inspectors to your plant. They check cleanroom conditions, equipment calibration, and record-keeping. A single violation can delay approval by months.
- Labeling Approval: Your label must say the same thing as the brand’s-no extra claims, no missing warnings.
- Post-Approval Monitoring: Even after approval, you must report any manufacturing changes, adverse events, or out-of-spec batches within 24 hours.
Why Quality Control Is Non-Negotiable
The FDA doesn’t trust luck. That’s why every facility must follow Current Good Manufacturing Practices (CGMP). These rules cover everything: air quality (ISO Class 5-8 cleanrooms), employee hygiene, equipment cleaning, and data integrity. You can’t just write down numbers-you must have electronic logs that can’t be altered. The most common inspection failures? Three big ones:- 37% of warning letters cite failure to investigate out-of-spec results
- 29% point to inadequate process validation
- 24% flag weak quality unit oversight
Complex Generics: The New Frontier
Not all generics are equal. Simple pills-like metformin or atorvastatin-are easy to copy. But complex drugs? That’s where things get hard. Topical creams, inhalers, nasal sprays, and extended-release tablets have delivery mechanisms that are nearly impossible to replicate with standard testing. A 2022 case study showed one manufacturer spent 7 years and $47 million just to match the skin absorption of a generic corticosteroid cream. Traditional bioequivalence studies didn’t predict real-world performance. That’s why the FDA launched its Complex Generic Products Initiative. As of 2023, they’ve published 127 product-specific guidances to help manufacturers navigate these challenges. The number of complex generics in development has jumped from 12% in 2015 to 35% today.
Market Realities: Cost, Competition, and Supply Chains
Generic drugs make up 90% of U.S. prescriptions but only 19% of drug spending. That’s over $1.7 trillion saved in the last decade. Yet, the economics are brutal. For simple generics, 15-20 companies may compete. Prices drop 70-80% within two years. Many manufacturers can’t survive. That’s why 78% of active pharmaceutical ingredients (APIs) now come from just two countries: China and India. The FDA has been inspecting these facilities more often-but supply chain risks remain. On the flip side, complex generics face only 2-5 competitors. Prices drop slower, margins stay higher, and manufacturers can invest in better tech. Some brand-name companies even produce their own “authorized generics,” selling them under a different label right after their patent expires.What’s Next? AI, Digital Twins, and Continuous Manufacturing
The industry is changing fast. The FDA has approved 17 facilities using continuous manufacturing, where drugs are made in one flowing process instead of batch-by-batch. Vertex’s cystic fibrosis drug, made this way, hit 99.98% batch acceptance-far better than the 95% average from traditional methods. Pfizer’s pilot program using AI to scan tablets for defects cut visual inspection errors by 40%. “Digital twins”-virtual models of manufacturing lines-are being tested to predict failures before they happen. The future isn’t just about making cheaper pills. It’s about making them smarter, safer, and more reliable.Are Generic Drugs Safe? The Evidence
A 2023 survey by the Association for Accessible Medicines found 89% of pharmacists have high confidence in generic quality. Only 3% reported noticeable differences in patient outcomes. That doesn’t mean there are no risks. For drugs with a narrow therapeutic index-like warfarin or levothyroxine-even small variations can matter. But the FDA’s strict bioequivalence rules and ongoing monitoring keep these cases rare. The real story? Generics save lives by making treatment affordable. A generic version of Sovaldi (sofosbuvir) dropped hepatitis C treatment from $84,000 to $28,000 per course. Without generics, millions couldn’t afford care.Are generic drugs as effective as brand-name drugs?
Yes. The FDA requires generic drugs to have the same active ingredient, strength, dosage form, and route of administration as the brand-name version. They must also prove bioequivalence-meaning they deliver the same amount of drug into the bloodstream at the same rate. Studies show no meaningful difference in effectiveness for the vast majority of patients.
Why do generic drugs look different from brand-name drugs?
U.S. trademark law prohibits generics from copying the exact appearance of brand-name drugs to avoid confusion. So, generics may differ in color, shape, size, or flavoring. But these changes are only in inactive ingredients and don’t affect how the drug works.
Can generic drugs have different side effects?
The active ingredient is identical, so side effects should be the same. However, differences in inactive ingredients (like dyes or fillers) may cause rare allergic reactions in sensitive individuals. If you notice a new reaction after switching to a generic, talk to your doctor or pharmacist.
How long does it take to get a generic drug approved?
For simple generics, the FDA aims to review applications within 10 months under current rules (GDUFA IV). Complex drugs, like inhalers or extended-release tablets, can take up to 36 months due to additional testing and scrutiny.
Why are most generic drugs made in China and India?
Manufacturing costs are significantly lower there, and these countries have invested heavily in FDA-compliant facilities. As of 2023, 78% of active pharmaceutical ingredients (APIs) used in U.S. generics come from China and India. The FDA inspects these facilities regularly, but supply chain dependence remains a concern.



Ethan Zeeb
March 3, 2026 AT 12:08They don't tell you this, but the real bottleneck isn't the science-it's the paperwork. I worked in pharma compliance for six years. The ANDA isn't just an application, it's a full-time job for a team of lawyers, chemists, and auditors. One typo in a batch log can delay approval for months. And don't even get me started on how they audit electronic records. You think your Excel sheet is safe? Nah. They check the metadata. Every edit. Every deletion. You can't even fix a decimal without a trail.
That’s why so many small manufacturers just give up. It’s not about quality-it’s about surviving the bureaucracy.
Jane Ryan Ryder
March 5, 2026 AT 04:54So let me get this straight-we spend billions to make pills that look different but work the same, all because some lawyer in 1982 decided generics shouldn’t look like the real thing? Classic American nonsense.
Just make them look identical and save everyone the headache. Who cares if the packaging’s different? You’re not buying a Nike sneaker-you’re buying a pill that lowers your blood pressure. Let people take the cheap one without the shame.
Chris Beckman
March 5, 2026 AT 19:54wait so if the active ingredient is the same why do some generics make me feel weird? i switched from brand to generic for my thyroid med and i swear i felt like a zombie for 3 weeks. my doc said 'it's all in your head' but i know better. the excipients gotta be different and some people are sensitive to corn starch or whatever. they don't test for that. they just test for the drug. that's insane. people die from this. i'm not exaggerating.
also why do they use gelatin in capsules? what if you're vegan? no one asks. this whole system is built on convenience not care.
Darren Torpey
March 7, 2026 AT 19:51Man, this whole process is like watching a symphony where every instrument has to hit the exact note-or the whole thing collapses. One grain of lactose out of alignment and suddenly your tablet doesn't dissolve. It’s not magic. It’s not luck. It’s precision engineering on a molecular level.
I used to think generics were just cheap knockoffs. Now I see them as silent heroes. The unsung lab techs in India, the FDA inspectors in Ohio, the engineers tweaking drying temps at 3 AM-all of them keeping millions of people alive while the rest of us scroll through memes. We don’t thank them. We should.
Also-AI scanning tablets? That’s next-level. Imagine a robot with a magnifying glass, staring at 10,000 pills a minute, looking for a flaw the human eye would miss. That’s not automation. That’s art.
Richard Elric5111
March 8, 2026 AT 11:36One cannot help but observe the profound epistemological tension inherent in the regulatory framework governing generic pharmaceuticals. On one hand, we invoke the Kantian imperative of universalizability-i.e., if a drug is bioequivalent, it must be therapeutically equivalent. On the other, we permit qualitative heterogeneity in excipients, which, as a priori conditions of pharmaceutical efficacy, introduce a latent contingency into the therapeutic act.
Thus, the ANDA system functions not as a guarantee of sameness, but as a probabilistic approximation of equivalence, predicated upon statistical norms rather than ontological identity. In this light, the patient’s trust becomes not a rational conclusion, but an act of phenomenological faith.
Betsy Silverman
March 8, 2026 AT 21:28I love how this post breaks down the science without making it feel like a textbook. Seriously, kudos.
My mom’s on warfarin, and we switched generics last year. She was terrified. I sat with her, read the FDA’s bioequivalence guidelines together, and we even called the pharmacy to ask which manufacturer made the new batch. Turns out it was the same one as before-just a different label.
People don’t realize how much trust goes into this. It’s not just chemistry. It’s trust in systems we never see. I’m glad someone took the time to show how rigorously it’s all monitored. It’s reassuring.
Ivan Viktor
March 9, 2026 AT 09:47So China and India make 78% of our drug ingredients and we’re okay with that? Cool. Cool cool cool. Just don’t mention the part where the FDA inspector gets food poisoning from the local water during inspections. That’s not in the brochure.
Also, why is the FDA’s review time 10 months for simple generics? That’s longer than it takes to get a new iPhone. And we’re supposed to be grateful?
Zacharia Reda
March 11, 2026 AT 01:19Okay, but the real villain here isn’t the manufacturers-it’s the patent trolls. Brand companies extend their monopolies by tweaking a pill’s coating or delivery system just enough to file a new patent. Then they slap a ‘new formulation’ label on it and jack up the price. Meanwhile, the generic makers are stuck waiting for legal clearance.
That’s why complex generics are so rare. It’s not because they’re hard to make. It’s because the legal system is rigged. If we fixed patent abuse, we’d have 10x more generics on the market. And prices? They’d drop to pennies.
Also-continuous manufacturing? That’s the future. Batch processing is like using a typewriter in 2024. Time to upgrade.
tatiana verdesoto
March 11, 2026 AT 07:35My cousin works at a generic drug plant in Indiana. She told me they have to retest every single batch of lactose because suppliers change. One time, a new batch had slightly higher moisture-and 30,000 tablets had to be scrapped. They cried. Not because of the cost, but because they knew someone was waiting for those pills.
Generics aren’t just cheaper. They’re more human than you think.